Lisa A. Pierson, DVM
Hyperthyroidism is a very common endocrine disorder of older (usually >10 years of age) cats. In fact, it is said to be the most common endocrine disorder in cats but judging by the large volume of emails I receive asking for help with feline diabetes management, I would say that it is a toss-up as to which disease is more common.
The catalyst for the writing of this webpage is the recent introduction to the veterinarian-prescribed diet market of Hill’s y/d which is an iodine-deficient diet targeted at feline hyperthyroid patients.
Please note that Hill’s has made false and misleading statements about this diet that will be addressed below.
What are the signs of hyperthyroidism?
What are the causes of hyperthyroidism?
How is hyperthyroidism diagnosed?
What are the treatment choices of hyperthyroidism?
-
Hill’s y/d – an iodine-deficient canned and dry food
Comments on hyperthyroidism and chronic kidney disease (CKD)
What is hyperthyroidism?
Hyperthyroidism results from an overproduction of thyroid hormones (mainly T4) from a tumor in the thyroid gland. This tumor, in over 97% of all cases, is a benign (non-cancerous) adenoma.
To repeat, hyperthyroid patients do not have cancer except in very rare (2-3%) cases where a thyroid carcinoma is the cause of the disease.
An elevation in thyroid hormones increases the metabolic rate of the body which puts stress on the heart, kidneys, nervous system, gastrointestinal tract, liver, as well as all other organs of the body.
Think of how hard your car’s engine has to work and how much fuel it uses if you rev up the motor (increase its rpms) by stepping on the gas pedal while in neutral.
This is what is happening inside your hyperthyroid cat’s body. Every organ system is under the negative influence of an abnormal increase in the body’s metabolism.
In the analogy above, food is your cat’s fuel and it is being used at a faster rate than normal which results in an increased hunger and weight loss.
Hyperthyroidism is eventually fatal if left untreated.
What are the signs of hyperthyroidism?
Since elevated thyroid hormones negatively affect every organ system in the body, the clinical signs are extremely varied but include some or all of the following – with an increased appetite and weight loss being the two most common:
- increased appetite (but sometimes decreased)
- weight loss (fat and muscle) in the face of a good appetite
- increased activity (“acting like a kitten again”)
- increased drinking and urination
- vomiting
- diarrhea
- heart disease – increased heart rate/’pounding’ heartbeat
- increased respiration rate
- hair coat/skin/nail abnormalities
- nighttime yowling/restlessness/confusion/behavior changes
- high blood pressure (hypertension) – Please note that if your cat’s eyes look like big black pools (dilated pupils), this is a sign of possible retinal detachment which can occur secondary to high blood pressure and will result in partial or total blindness. Not all hyperthyroid cats become hypertensive but is a good idea to have your veterinarian monitor your cat’s blood pressure.
What are the causes of hyperthyroidism?
I wish we knew the definitive answer to that question.
Possible causes of hyperthyroidism include:
- Iodine levels in cat food – either too low or too high. Note that this is a very poorly regulated nutrient in cat food with levels varying over a 30-fold range.
- PBDEs – PBDEs are fire retardant chemicals that can be found in high concentrations in some fish and also in house dust. Since PBDEs are known to affect thyroid function, and cat foods tend to be high in fish, there may be a causal link between hyperthyroidism and fish consumption. This is one of several reasons why I recommend against feeding fish-based diets to cats.
- Soy in cat food – Soy is a known disruptor of thyroid gland function. If you have read my Feeding Your Cat: Know the Basics of Feline Nutrition which outlines what it means to be an obligate carnivore, you will understand that soy has no logical place in cat food. However, soy will increase the profit margin for pet food companies. Therefore, it is present in many cat foods – especially those made by Purina.
According to one study, soy was identified in 60% of all tested cat foods at a level high enough to interfere with thyroid function.
- BPA (bisphenol A) – BPA is a known endocrine disrupter that may play a role in the cause of hyperthyroidism. BPA is found in the coating of the inside of some cans of pet food. Generally speaking, the smaller (3 ounces and 5.5 ounces) cans will be less apt to contain BPA than the larger (12-13 ounce) cans.
How is hyperthyroidism diagnosed?
Your veterinarian will perform a thorough physical exam including palpating (feeling) both lobes of the thyroid gland which sit in the throat area near the Adam’s Apple. A normal thyroid gland should not be large enough to feel whereas an adenomatous thyroid gland will usually be large enough to palpate.
Next, a full blood panel, cbc (complete blood cell count), and urinalysis will be performed to look for any disease process(es) that could explain any of the clinical signs that your cat is exhibiting.
It is important that the blood panel include a total T4 level since this is the most important value to look at when assessing thyroid gland health. The panel that your vet chooses may also include a free T4 which is also useful in diagnosing some hyperthyroid patients but is not as clearly interpreted as total T4. Free T4 can be falsely elevated for various reasons.
The panel that I choose to use for my patients includes both total T4 and free T4 but panels vary from lab to lab.
Thyroid scintigraphy (thyroid scan) is considered the ‘gold standard’ for diagnosing mild hyperthyroidism but it is not readily available to most people. However, as noted below, the best treatment for hyperthyroidism is radioactive iodine and, if available, you should choose a facility that performs thyroid scintigraphy to characterize the size, shape, and location of the abnormal tissue in order to gain more knowledge of the disease severity and to also aid in selecting the proper dosage of I-131.
What are the treatment options for hyperthyroidism?
In the sections below, you will see links to Insights into Veterinary Endocrinologywritten by Dr. Mark Peterson, DVM, DACVIM. Dr. Peterson is a world renowned expert in feline hyperthyroidism and was the first veterinarian to recognize this condition in the early 1970s. He has treated over 10,000 hyperthyroid cats in the past 30 + years and has lectured countless times to veterinarians from all over the world regarding topics in endocrinology.
Dr. Peterson and I have collaborated recently regarding the new Hill’s diet, y/d, and on other general nutrition issues. In combining our individual strengths (Dr. Peterson’s background in endocrinology and mine in nutrition), Dr. Peterson has written several very informative blog entries.
~~~~~~~~~~~~~~~~~~~~~~~~
There are 4 treatment options for hyperthyroidism:
- radioactive iodine (I-131) – the ‘gold standard‘
- anti-thyroid medication (e.g. methimazole)
- surgery
- Hill’s y/d (a diet deficient in iodine – canned and dry)
Note that only radioactive iodine and surgery address the underlying cause of the disease which is a tumor.
Anti-thyroid medication and an iodine-deficient diet do not address the tumor which will continue to grow.
Therefore, representatives from Hill’s are making a false statement when they claim that y/d “restores thyroid health.”
~~~~~~~~~~~~~~~~~~~~~~~~~~
Radioactive iodine – 131 (I-131)
Radioactive iodine is the treatment of choice for hyperthyroidism in nearly all cases. This treatment involves an injection of a very small dose of radioactive iodine that is placed just under the skin. Because the thyroid gland heavily concentrates iodine, the thyroid tumor will be selectively destroyed.
In addition to the thyroid tumor being targeted, any other ectopic (found somewhere other than its normal location) overactive thyroid tissue will also be destroyed. This ectopic tissue is often located in the chest cavity but will show up on a thyroid scan as discussed below.
A small risk (~5%) of hypothyroidism (the opposite of hyperthyroidism) exists if too much normal tissue is also destroyed. These cats will need to receive thyroxine supplementation temporarily or for life.
On the flip side, a small number of cats (~5%) remain hyperthyroid (and require a second treatment) if not enough of the adenoma is destroyed or if the patient actually has a carcinoma (cancer) instead of a benign adenoma. In the case of a carcinoma, a much higher dosage of I-131 is needed to effectively treat the disease.
As noted above, a thyroid scan (scintigraphy) helps the clinician determine the size, shape, and location of the abnormal tissue which helps determine the proper dosage of I-131 to ensure the best possible outcome.
Without a scan, the dosage will only be a guess.
Other treatments are discussed below but I can say without hesitation that if any of my own deeply-loved cats ever ended up with hyperthyroidism, this would be the only treatment that I would consider.
Update: 6 months after I wrote the statement above, my Andy had a slight-to-moderate rise in his T4 and was showing clinical signs of hyperthyroidism – weight loss and agitation/restlessness – especially at night. I took him to our local imaging clinic and had him scanned. Right arrow = normal; Left arrow = thyroid adenoma.
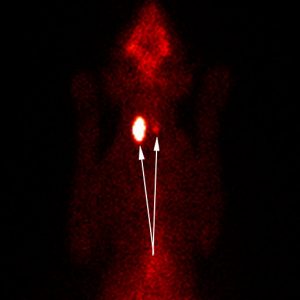
Andy was admitted to the clinic on Sunday. He was scanned that day and received his I-131 injection on Monday. He was able to come home on Thursday.
Was he miserable? Yep. Was I stressed and anxious? You bet. But now I have my Andy back. He has gained 1.5 lbs and, at 16 years of age, is doing great.
Many people worry about the hospital stay and the stress that it will cause for the cat. Yes, it is stressful but the benefits far outweigh the difficult few days and it sure beats having to give a pill (methimazole) twice daily, for the rest of the cat’s life, which is a medication that can have significant side effects and does not address the tumor. More on this drug below.
~~~~~~~~~~~~~~~~~~~~~~~~~~
Anti-thyroid medication:
methimazole (Tapazole and Felimazole)
carbimazole is a newer drug that is rarely used and not readily available in the United States.
These drugs are known as ‘anti-thyroid’ medications since they interfere with the thyroid gland’s production of thyroid hormones.
I will say at the outset of this section on anti-thyroid drugs that I am not a fan of putting any chemical into my own body, or that of my own cats or patients. For every positive action that a drug exerts on a living being, there are plenty of side effects that are very often overlooked by the doctors prescribing the medications.
There are many cats that do well on these drugs but side effects are not uncommon and include nausea, vomiting, and severe allergic/itchy facial skin reactions and, less frequently, life-threatening liver dysfunction, bone marrow disease, and bleeding problems.
While these drugs effectively lower the thyroid hormones and ameliorate the clinical signs of hyperthyroidism, they do not address the underlying tumor and, therefore, the tumor will continue to grow with the risk that it will become a malignant cancer over time.
As the tumor continues to grow, the dosage will often need to be raised which means that the patient must be monitored with periodic blood tests for life. The frequency will depend on the patient but as we all know, trips to the veterinarian are expensive and very stressful for the patient.
Other health factors may necessitate lowering the dosage. Therefore, lab monitoring is very important for these patients.
If methimazole is chosen over I-131, I strongly prefer the transdermal preparation which is a cream that is applied to the ear. This formulation results in less gastrointestinal (vomiting/diarrhea) side effects when compared to the pill form.
Plus, it is a much more humane and less stressful way to administer the medication.
If the pill form is used, please see my Pilling Cats article and never, ever ‘dry pill’ any medication for any cat or dog. All pills or capsules need to be ‘chased’ with food or at least 4 mls of water via a syringe.
Or, better yet, use Pill Pockets as discussed on the Pilling Cats page.
At first glance, I-131 may appear to be a more expensive treatment but in many cases it turns out to be less expensive when compared to lifelong treatment with methimazole when the cost of the medication and the continued monitoring are considered.
Also, the hassle of twice-daily medication must be considered.
In the end, however, I-131 is closer to being a true cure for this disease than methimazole since it addresses the underlying tumor.
Note that if your cat has been on methimazole and you now want to have him treated with I-131, you may have to withdraw the methimazole for ~1-2 weeks prior to I-131 treatment.
For more information on these drugs, please see Dr. Mark Peterson’s discussion here.
~~~~~~~~~~~~~~~~~~~~~~~~~~
Surgery
Surgery to remove the thyroid adenoma has fallen out of favor since I-131 became available. This is true for several reasons:
1) It is impossible to differentiate normal tissue from tumor tissue. If both lobes of the gland are involved and removed, this will result in hypothyroidism necessitating lifelong treatment with thyroxine.
2) The parathyroid gland which sits right next to the thyroid gland can be damaged or accidentally removed. The parathyroid gland is critical for calcium balance in the body and if damaged or removed, serious complications, including death, can result.
3) General anesthesia is necessary which is always a risk but even more so in an older patient with hyperthyroidism considering how many organs are negatively affected by this disease. Severe heart disease can be present in these patients especially if they have been hyperthyroid for a long time. Any level of heart disease will increase the risk associated with anesthesia. For this reason, if surgery is the treatment of choice, it is recommended to stabilize the patient with anti-thyroid medication prior to the surgery.
4) Some hyperthyroid cats have ectopic (not in the normal location) thyroid adenoma or carcinoma tissue located in the chest cavity which the surgeon will not be able to remove. Plus, the surgeon will not even be aware of its presence unless a thyroid scan was performed.
See here for a more comprehensive chart comparing the pros and cons of each of the 3 treatments discussed above.
~~~~~~~~~~~~~~~~~~~~~~~~~~
Hill’s y/d
This iodine-deficient diet is the newest addition to the Hill’s ‘alphabet prescription diet’ product line and it is targeted at the feline hyperthyroid patient. As stated above, representatives of the Hill’s company have made false and misleading statements about this diet that will be addressed below.
y/d is formulated to be deficient in iodine with the simple goal of providing less ‘building material’ for the patient’s thyroid tumor and normal glandular tissue to make thyroid hormones (T3 and T4). Iodine is an important component of these hormones withT3 needing 3 iodine atoms and T4 containing 4 iodine atoms.
The premise of this diet is simply to starve the thyroid gland of iodine but here is where the issue of ‘tunnel vision’ nutrition comes into play.
While starving the thyroid gland of iodine, the entire body – including the thyroid gland itself – is also negatively affected by this deficiency.
~~~~~~~~~~~~~~~~~~~~~~~~~~~~
If anybody reading this has not read at least the first part of my Feeding Your Cat: Know the Basics of Feline Nutrition article, I will briefly summarize it here because, before reading my comments about y/d, it is important to understand what constitutes a healthy diet for a cat.
In a nutshell, the cat is an obligate carnivore which means:
- They are designed by nature to get their protein from other animals (meat), not plants (grains/potatoes/other vegetables).
- They lack the enzymes necessary to efficiently process carbohydrates.
- They have a low thirst drive and are designed to get their water with their food. This means that there is no dry food that is suitable to feed to a cat.
Their normal prey is ~70% water and in times of drought, they could actually survive on the moisture in their prey. Canned foods are ~78% water and dry foods are only ~8-10% water.
Several studies have shown that the water intake and urine output of cats fed canned food are double that of dry food-fed cats. This is taking into consideration all sources of water from the food and the water bowl.
Please understand that a cat on a dry food diet will drink much more water from a bowl than a canned food-fed cat but he will not make up the deficit caused by the feeding of a water-depleted diet of dry food.
Considering that water is one of the most important nutrients for every living creature, it is easy to understand why it is much more physiologically sound to feed canned food diets to cats rather than dry food.
See Urinary Tract Health for some graphic pictures of what happens to cats like Opie when fed a water-depleted diet.
~~~~~~~~~~~~~~~~~~~~~~~~~~~~
Summary statement regarding y/d:
I would only use this diet if:
- I-131 was not available or the client could not afford the treatment, or
- the patient was not a good candidate for surgery, or
- the patient had shown an intolerance to transdermal methimazole.
In other words, I see y/d as a last resort and certainly not a first-line treatment.
Why?
Because:
- y/d leaves the whole body in a state of iodine deficiency. This is an excellent example of tunnel vision nutrition – i.e.- only paying attention to the thyroid gland, in this case, and not the rest of the body. Safety studies have not been conducted to assess the long-term damage to the body when left in an iodine-deficient state.
Most of our knowledge of iodine centers around the thyroid gland but there is strong evidence pointing to iodine as playing an important role in immune health, adrenal function, breast health, and also having antioxidant properties.
- y/d does not address the disease process (tumor) that is causing the hyperthyroidism and the tumor will continue to grow. Therefore, it does not “restore thyroid health” as claimed by Hill’s.
The longer the tumor is allowed to grow, the higher the chance of it becoming a malignant carcinoma.
- y/d is too low in protein for many cats especially considering the muscle-wasting state that hyperthyroid cats are already in. (See Dr. Peterson’s article here.)
- y/d is too high in carbohydrates. (See Diabetes) Note that many hyperthyroid cats have sub-clinical diabetes. Feeding them a high carbohydrate diet could very well tip them over the edge into overt diabetes.
canned y/d: 24% carbohydrate calories
dry y/d: 23% carbohydrate calories
mouse: 1-2% carbohydrate calories
- dry y/d has an extremely unhealthy ingredient list for an obligate carnivore and it is water-depleted. (See Urinary Tract Health.)
Corn Gluten Meal, Animal Fat (preserved with mixed tocopherols and citric acid), Whole Grain Corn, Soybean Mill Run, Dried Egg Product, L-Lysine, Chicken Liver Flavor,…..
Please read the above ingredient list with your cat’s obligate carnivore status in mind. Also understand that your hyperthyroid cat needs a high amount of high quality protein since the disease is causing his body to ‘eat’ (catabolize) his own muscle mass.
Corn is not a “high quality” protein for a carnivore.
I would never feed a diet like dry y/d to any cat in my care. It is a more appropriate diet for a horse or a cow to be eating. Please note that there is no meat in this food. The only animal-based protein is the dried egg product which is lower on the list than even the fiber source so there is next-to-nothing in the way of animal protein in this diet.
- y/d canned has a better ingredient list than the dry and is at least a properly hydrated diet but note that liver is the first ingredient after water. Liver is high in vitamin A and a diet of predominantly liver does not represent a species-appropriate balance of nutrients. However, note that liver is cheap and provides a higher profit margin for the company.
Water, Liver, Meat by-products, Chicken, Whole Grain Corn, Rice Flour, Chicken Fat (preserved with mixed tocopherols and citric acid), Chicken Liver Flavor, Powdered Cellulose,…..
See Dr. Peterson’s article: Is Hill’s y/d a Nutritious Diet for Hyperthyroid Cats?
If you choose to feed this diet, please feed the canned version and not the dry.
- The patient cannot be allowed to eat any other food which means no treats of any kind. He must eat only y/d which can pose a problem in multiple-cat households or if he suddenly stops eating the food.
- This diet cannot be fed to non-hyperthyroid cats. Hill’s states that it can be fed to normal cats if these cats are also fed some regular food. However, I would not subject your healthy cat to this diet with the hope that you feed enough food from another source to meet his iodine needs – especially in light of the fact that there are diets on the market that are very low in iodine – too low to furnish enough iodine to make up for the bulk of the diet being iodine-deficient.
In my strong opinion, Hill’s is being very irresponsible when making the recommendation to: “supplement (y/d) with 1 tablespoon of regular cat food (dry or canned) each day to provide additional iodine”. Given the wide range of iodine in commercial cat food, this recommendation will not ensure adequate iodine in every healthy cat that may be subjected to y/d as the bulk of their diet.
- There is compelling scientific evidence to show that feeding an iodine-deficient diet can actually make the hyperthyroid patient worse over time.
When there is not enough iodine in the body, thyroid hormones decrease. This signals the pituitary gland to secrete TSH (thyroid stimulating hormone). TSH’s action on the thyroid gland causes it to grow larger (hypertrophy/goiter).
Thyroid Response to Low Intake of Iodine:
- Deficient dietary iodine intake causes the thyroid gland to make less T4
- Plasma T4 levels drop
- This results in increased TSH release from the pituitary gland
- leading to increased iodide trapping in the thyroid gland to maintain T3 secretion
- resulting in thyroid hypertrophy due to increased TSH release = GOITER
If you are interested in learning more about the biochemistry of iodine deficiency and thyroid disease, see Dr. Peterson’s article: Does Iodine Deficiency Cause Thyroid Disease in Cats?
Reminder: y/d is an iodine-deficient diet.
Here is an excerpt from Dr. Peterson’s article:
So, based on the trend to lower iodine levels in cat food over the last two decades, could iodine deficiency be contributing to the explosion in hyperthyroid cases that we are seeing today?
In support of that reasoning, a recent case-control study reported that cats consuming commercial foods which were relatively deficient in iodine were more than 4 times as likely to develop hyperthyroidism compared with cats that ate iodine-supplemented foods.”
…and another excerpt from Dr. Peterson’s article under the heading:
Could y/d make this situation worse?
…..will lowering T4 and T3 secretion in these hyperthyroid cats lead to increases in circulating TSH and continued stimulation of thyroid growth and proliferation in some cats? Will this TSH stimulation cause transformation of benign adenomatous thyroid tissue to carcinoma, as has been documented to occur in some hyperthyroid cats?
The short answer is this: we simply do not know. The long-term safety studies needed to answer this question have not yet been done.
Because Hill’s y/d is not a drug (although it’s certainly being marketed as a replacement for methimazole), the company is not required to do the these safety studies, and it’s fairly clear that they have no intension of paying to have them done.”
Also note this excerpt from an article that appeared in the Journal of Feline Medicine and Surgery (2010) entitled Feline Hyperthyroidism: Potential relationship with iodine supplement requirements of commercial cat foods:
Feline hyperthyroidism resembles toxic nodular goiter (TNG) of humans with discrete foci of benign adenomatous hyperplasia. The etiology of TNG includes iodine deficiency and consumption of or exposure to goitrogens in food, water, and the environment.”
The article goes on to discuss evidence that the current NRC dietary minimum iodine requirement of 1.4 ppm may be too low and may be contributing to feline hyperthyroidism.
Note that y/d is a very iodine-deficient diet at 0.2 ppm (range 0.1 – 0.3 ppm) and we know that iodine-deficient diets cause goiter.
~~~~~~~~~~~~~~~~~~~~~~~~~~~
Is Hill’s being truthful in their marketing claims? Are they considering what is best for your hyperthyroid cat?
You be the judge.
- Hill’s states that this diet “restores thyroid health”. After reading the information above, I hope that you can see that this is a blatantly false statement.
Hyperthyroidism is caused by a benign thyroid gland tumor. Feeding a diet that is deficient in iodine is not halting the growth of the tumor.
In addition, it has been common knowledge for many years that diets deficient in iodine cause goiter (thyroid gland enlargement).
The tumor will keep growing unless addressed with I-131 or surgery. This continued growth will only enhance the chances of the benign tumor becoming cancerous.
Therefore, it should be very clear that this diet does not “restore thyroid health.”
- Hill’s is calling this an “iodine-restricted” diet and claiming that it is “not iodine-deficient” which is in direct contradiction to their own study as well as studies of other researchers who have investigated the dietary iodine needs of the cat.
To illustrate why their statement is false:
There are studies showing that the minimum iodine requirement in cat food should be 1.4 ppm. In fact, the current NRC requirement states a minimum of 1.4 ppm.
A Hill’s study using a corn-based diet stated that the minimum iodine requirement was 0.46 ppm.
y/d is 0.2 ppm (range 0.1 – 0.3 ppm)
How can Hill’s perform a study coming up with 0.46 ppm as a minimum requirement and then state that a diet with less than half that amount is “not iodine-deficient”?
Here is what Dr. Mark Peterson has to say about this issue in his blog entry entitled Treating Hyperthyroid Cats with an Iodine Deficient Diet (Hill’s y/d): Does It Really Work?
“Hill’s y/d is clearly an iodine deficient diet, containing levels of approximately 0.2 mg/kg (0.2 ppm) on a dry matter basis, well below the minimum daily requirement for adult cats (0.46 mg/kg or 0.46 ppm) of food. It’s important to note that the study that established this minimum daily requirement for cats was done by investigators funded by Hill’s Pet Nutrition. So, claims that this is just a low iodine diet, but not one deficient in iodine is nonsense, unless one does not believe the results of that study.”
An important issue regarding the Hill’s iodine study is that they fed the test cats a corn-based diet. No nutrient is an island unto itself. All nutrients are influenced by other nutrients in the diet. Therefore, it only makes sense to feed a cat a species-appropriate diet (which corn is not) when trying to figure out the optimal level of any nutrient in the diet.
Since Hill’s is known for manufacturing feline diets with high levels of species-inappropriate ingredients to enhance their profit margin, it was not the least bit surprising to learn that their iodine study involved feeding cats a corn-based diet.
Did this skew the results? We have no way of knowing but, again, if you are going to conduct any nutrient study, common sense dictates that you at least feed the test subjects a species-appropriate diet which, in this case, would be meat – not corn.
- This statement is appearing in our veterinary journals:
“Managing hyperthyroidism is now as easy as feeding your cat,” says Dru Forrester, DVM, MS, Dipl. ACVIM, director of Scientific & Technical Communication for Hill’s Pet Nutrition.
This irresponsible and misleading marketing is going result in far fewer cats receiving the gold standard treatment of I-131.
It is natural for all of us to want to take the easy (and cheaper) way out and this inherent desire is exactly what the Hill’s marketing team is focusing on as is evident by Dr. Forrester’s statement above. However, ‘easy’ is not always ‘healthy.’
~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~
Comments on treating hyperthyroid patients that also have CKD (chronic kidney disease):
Since hyperthyroidism and kidney disease are common problems in older cats, it should come as no surprise that many hyperthyroid patients also have concurrent kidney disease. It is estimated that 30-35% of all hyperthyroid cats also have some level of kidney disease.
However, the increased metabolic rate of the hyperthyroid patient can make the kidneys looking better ‘on paper.’ This is because an elevated metabolic rate causes an increase in blood flow/increase in pressure through the kidney which makes it filter out waste products (e.g., BUN and creatinine) more efficiently.
When the patient’s T4 level is returned to normal – regardless of treatment choice – underlying kidney disease may be unmasked.
It is very important to understand that treating the hyperthyroid state did not cause kidney disease.
In addition to the increased blood flow making the patient’s lab values look better than they might end up being post-treatment for hyperthyroidism, hyperthyroid cats have less muscle mass than healthy cats and since creatinine comes from internal muscle breakdown (a normal daily occurrence), a skinny kitty is going to generate less creatinine – making his kidneys look better than they really are.
Once the treated hyperthyroid cat starts to regain his muscle mass, the creatinine value may rise – leading the clinician to erroneously assume that the kidneys have worsened.
Again, the underlying kidney disease is being masked by the hyperthyroidism but it is critical to understand that treating a cat for hyperthyroidism does not actually cause kidney disease.
Quite the contrary.
Recent research has shown that the negative effects (including the increase in blood pressure at the kidney level) of an increased metabolic rate may very well contribute to the development and progression of kidney disease in the untreated hyperthyroid cat.
While it may be tempting to leave a hyperthyroid cat either untreated or undertreated with very low levels of anti-thyroid medication, this can have a negative effect on kidney health, as well as heart health.
Many veterinarians shy away from I-131 or surgery versus anti-thyroid medication and Hill’s y/d because the first two are permanent and the last two are temporary. Their argument is that the medication dosage can be lowered or discontinued and the diet can be changed if they don’t like how the kidney values look once the T4 is lowered to the normal range.
But the idea of lowering the dosage of an anti-thyroid medication or altering the diet to let the patient ‘run hot’ so that the kidneys look better is not without its very unhealthy consequences.
Remember that hyperthyroidism is revving up your cat’s ‘engine’ (metabolic rate) damaging the entire body, including the kidneys.
The heart is another vital organ that suffers with this disease since it is basically wearing itself out by its increased rate of pumping.
I try very hard not to fall into the trap of ‘tunnel vision’ medicine. I focus on the whole body and, for that reason, I will repeat this statement:
I-131 is the only choice I will consider for my own cats.
If the I-131 unmasked kidney disease that was not apparent when their metabolic engine was in high gear, I would just deal with the CKD as needed.
Some readers may be familiar with a ‘methimazole (Tapazole) trial’ whereby the patient is put on this anti-thyroid medication to return the patient’s T4 level back to normal which often happens within 2-4 weeks. Once the T4 level is back to normal, the kidney values (BUN, creatinine, etc.) are assessed.
This trial is basically showing us what the kidney values will most likely be after effective I-131 treatment but in a reversible manner.
Even though this is definitely not the protocol that I would follow for my own cats – since I am going to treat their hyperthyroidism with I-131 no matter what their kidney values are – I do offer it as an option for my clients so that there are no surprises regarding kidney function after the I-131 treatment.
It is important for some clients to know what the kidney values may be after the T4 returns to a normal level but most of them forego the methimazole trial and go right to I-131 when hearing that this is how I treat my own cats.
I have never heard any client express regret for skipping the trial.
Note that the experts in this field who I have spoken with have recently tended toward slightly lower doses of I-131 for cats with significant kidney disease so that the T4 is more likely to end up in the upper part of the desired range versus the lower part. Therefore, please discuss the issue of dosage with the doctor administering the I-131 to your cat.
It must be understood that it is impossible to know the exact dosage that will result in your cat’s T4 ending up in the higher end of the desired range versus the lower end. Therefore, there is always a chance that a lower dosage of I-131 may not be enough to cure the hyperthyroidism and your cat’s T4 will still be too high. In these cases, the treatment will need to be repeated at additional expense.
September 2012
Updated October 2014
Updated November 2016
Lisa A. Pierson, DVM